into
Posted on: December 9, 2019
In the United Kingdom, the British National Formulary for Children is a national formulary which includes prescribing guidelines and drug monographs. You should read the relevant sections.
If possible, children should know why they need a medicine and be shown how they can take it. Young children and infants who cannot understand will usually take medicine from someone they know and trust – a parent or main carer. Therefore it is important that those who give medicines know about the medicine and how to give it. Occasionally, there may be problems in giving medicines – usually due to taste or difficulty swallowing a tablet or capsule. Parents or carers should not give in to fractious children and should not give medicines, as then compliance may be a problem; at all stages, the child should be comforted and reassured. The child must not be left with the impression that being given medicine is a punishment for being sick.
Another problem is that the child may seem better so parents/carers may not complete treatment, as in antibiotics. The approach depends on the child’s understanding and the circumstances:
• Under 2 years. Administration by parents if possible, using an approach which they believe is most likely to succeed.
• 2 to 5 year olds need a calm, gentle, firm, and efficient approach after they have been told what is happening. Play and acting out may help them understand. Rewards may encourage further co-operation.
• 5 to 12 year olds also need encouragement, respect for their trust, and an explanation attuned to their understanding.
• Over 12 years. At this age children must have a proper understanding of what is happening and share in the decision making as well as the responsibility. They must feel in control.
What children and carers need to know:
• The name of the medicine
• The reason for using it
• When and how to take it
• How to know if it is effective, and what to do if it is not
• What to do if one or more doses are missed
• How long to continue taking it
• The risks of stopping it
• The most likely adverse effects; those unlikely, but important; and what to do if they occur
• Whether other medicines can be taken at the same time
• Whether other remedies alter the medicine’s effect
Nursing staff involved with children need to remember about medicines and dosage problems in children.
Dosage Calculator
Most doses of medicines have been derived from trials or from clinical experience, and the nature of the drug should decide as to which method of dose calculation is the most appropriate. Drugs with a critical, narrow therapeutic index (i.e. a small difference between the effective and toxic dose), such as cytotoxics, require an accurate method – dosing based on body surface area. Using body surface area may be the most accurate method for dosing, as surface area better reflects developmental changes and function. However, the downside to this method is that it is not always easy, and it is time consuming to obtain accurate measurements for height and weight; so this is generally reserved for the potent drugs where there are small differences between effective and toxic doses.
Drugs with a wide therapeutic index (i.e. a large difference between the effective and toxic dose), such as penicillins, allow for some flexibility in dosing so an approximation is suitable – dosing based on a given dose or on a weight basis. A dose solely based on a weight basis (mg/kg) assumes that the dose is appropriate for a particular child or age. However, this may not be correct due to a variety of factors such as disease, prematurity or obesity. Also, remember that children grow at different rates, so a ‘one size fits all’ approach does not always apply. Before a dose is prescribed/given, appropriateness of the child’s weight and height should be re-assessed. Both methods rely on accurate weight and height measurements. Most drugs have a wide safety margin, so an alternative method of dosing is by age banding, and this is a much easier way of dosing. For example: paracetamol, the BNF for Children (2014–15) gives the following:
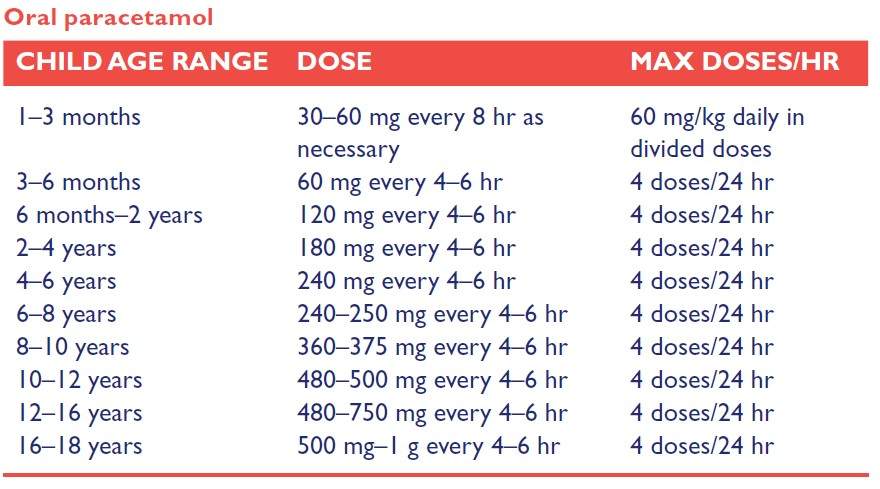
Once again, the appropriateness of the dose for the individual child, who may be small or large for their age, should always be assessed.
administered as well as aware of their responsibilities.



